Thyroid (Hypothyroidism)

Treatment Protocols for Hypothyroidism
Hypothyroidism occurs when the thyroid gland produces too little thyroid hormone when there is decreased conversion from T4 to T3, when there is an overproduction of reverse T3 (Wilson’s syndrome), or when the body is not efficiently using thyroid hormone. A large proportion of the population suffers some degree of hypothyroidism; however, the majority of those cases go undiagnosed.
Hypothyroidism can occur in either sex at any age, although middle-aged women are most commonly affected. The disease has a wide variety of symptoms, and they often reveal themselves slowly and subtly. Untreated, hypothyroidism can cause anaemia, a low body temperature and heart failure. There are many factors that influence thyroid dysfunction to see diagram below.
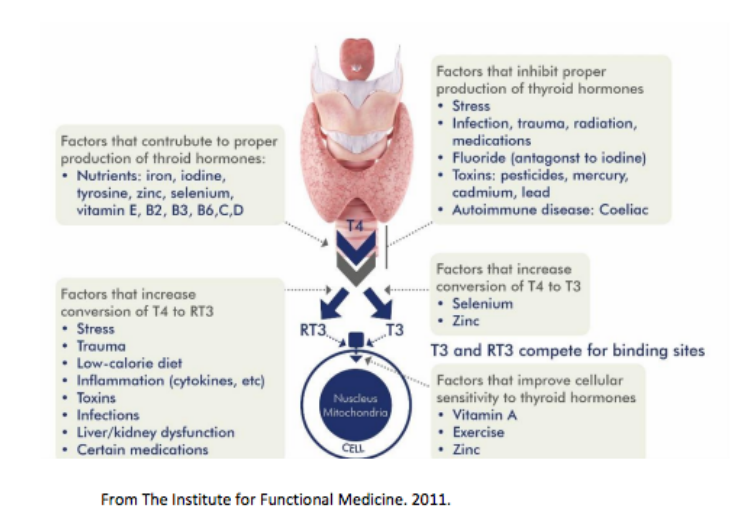
Hypothyroidism can take several forms, including:
- Hashimoto’s thyroiditis: this is the most common type of hypothyroidism. This is an autoimmune condition in which antibodies in the blood destroy tissues in the thyroid gland. As a result, the thyroid decreases in size and reduces its production of thyroid hormones.
- Post-therapeutic hypothyroidism: results from the treatment of hyperthyroidism with radioactive iodine or surgical removal of part or all of the thyroid gland. The treatment can leave the patient’s thyroid unable to produce sufficient amounts of thyroid hormone.
- Goitrous hypothyroidism: results from an extreme shortage of iodine in the diet, producing a goitre in the neck. It is relatively rare in the Western world due to the introduction of iodised salt.
Major factors that can contribute to hypothyroidism include:
- Chronic lack of iodine in the diet
- Inherited enzymatic defects
- Chronic stress and adrenal exhaustion
- Toxicity – the thyroid gland is very susceptible to toxins, especially toxic metals
- Positive family and/or personal history of autoimmunity
Common signs and symptoms of Hashimoto’s Thyroiditis include the following:
Firm, symmetrical enlargement of the thyroid gland that is not tender on palpation.
Goitre – Slow pulse – Lethargy – Hoarse voice – Slowed speech – Puffy face – Loss of eyebrows from the sides – Drooping eyelids – Intolerance to cold – Weight gain – Constipation – Dry, scaly, thick, coarse hair – Raised, thickened skin over the shins – Carpal tunnel syndrome – Confusion – Depression – Dementia – Headaches – Increased risk miscarriage – Menstrual cramps & menstrual disorders
Treatment for Hypothyroidism
Effective treatment involves supporting the thyroid gland with specific nutrients and herbal medicine where indicated. It food intolerances and/or dysbiosis (gut flora imbalance) are present they are significant barriers to treatment and need to be addressed.
- Support healthy thyroid function and energy production
- Minimise inflammation and oxidative stress
- Sensitise cortisol (interferes with thyroid hormone conversion) and manage mood and/or ongoing stress
- Investigate diet to reduce immune activation and support a healthy metabolism
Herbal Medicines, Diet, Specific Nutrients and LIfestyle factors play an important role:
- Herbal Medicines: Withania, Bacopa, Coleus, Barberry, St Mary’s Thistle, Kava, Rehmannia, St John’s Wort and others
- Nutrients: Zinc, Selenium, Iodine, Iron, Activated B Vitamins, Magnesium, Fat-soluble vitamins and others
- Probiotics (if dysbiosis present): Lactobacillus rhamnosus GG (LGG), L. Plantarum (299v) and others
- Diet: Anti-inflammatory diet, Identify food intolerances, low alcohol and caffeine, minimise processed foods
- Lifestyle: Activities that help relieve stress e.g. bushwalking, yoga, tai chi, meditation, relaxing baths. Regular exercise helps your body utilise thyroid hormone
- Toxins: Identifying toxin exposure and taking steps to avoid further exposure. Supporting detoxification and elimination pathways (herbal medicine and chelating substances)